BEST TREATMENT SPECIALIST FOR INFERTILITY
ପ୍ରାକୃତିକ ଉପାୟରେ ଅଣ୍ଡା ର ଗୁଣବତ୍ତା କେମିତି ବଢାଇବେ | Dr GSS Mohapatra on Infertility: Causes & Treatment in ODIYA
प्रेगनेंसी के लिए सबसे सही दिन When to get intimate ..Calculate Ovulation day
(LAPAROSCOPY, INFERTILITY, FIBROIDS & ENDOMETRIOSIS)
Infertility is defined as not being able to get pregnant despite having frequent, unprotected intercourse for at least a year for most people and six months if you are above 30 years of age. It can be that there is a cause in the female or male or both.
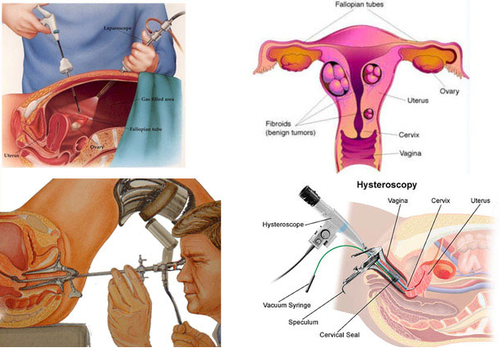
- it may be that there is an ovulation defect like PCOS ( polycystic ovarian syndrome) where hormones like testosterone and Prolactin are produced in excess.Block in the fallopian tube /damaged tube like hydrosalpinx which can result from conditions like adhesions,endometriosis and pelvic inflammatorydisease Congenital anomalies in the uterus / cervix like septate uterus, bicornuate uterus( 2 uterus, 2 cervix etc) or tumors in the uterine musculature ( Fibroids) which may distort the uterine cavity
where the endometrium grows outside the uterine cavity in sites like tubes and ovaries.This condition causes infertility, dyspareunia ( pain during coitus)
- CHOOSE THE RIGHT DOCTOR WHO UNDERSTANDS YOU AND YOUR PROBLEM
- CONCEAL NO FACTS. TELL HIM THE TRUTH
- HAVE FAITH IN HIS TREATMENT.
- GET THE TESTS DONE AND VISIT HIM AS AND WHEN CALLED
- LEAVE NOTHING TO CHANCE.
- FINALLY BELIEVE IN GOD BECAUSE IT IS MAN WHO PROPOSES BUT IT IS GOD WHO DISPOSES.
Both partners of an infertile couple should be evaluated
- Duration of infertility and results of previous evaluation and therapy.
- Menstrual history (cycle length and characteristics), which helps in determining ovulatory status.
- Medical, surgical, and gynecological history
- Personal and lifestyle history including age, occupation, exercise, stress, dieting/changes in weight, smoking, and alcohol use
- Sexual history, including sexual dysfunction and frequency of coitus. Infrequent or ineffective coitus can be an explanation
- Family history, including family members with infertility, birth defects, genetic mutations, or mental retardation.
Basic blood tests in females: s.tsh, s.prolactin, ESR,day 3 FSH,AMH ( especially in older females), s.oestradiol, s. Progesterone
It is an X ray done witha dye injected to know the status of the fallopian tubes, whether patent or not and it also gives an idea about the uterine cavity(Bicornuate/septate/arcuate)The diagnostic accuracy of hysterosalpingography is an area of considerable debate. Opsahl and coauthors evaluated the predictive value of the hysterosalpingogram (HSG) in the diagnosis of tubal and peritoneal factors.2 As expected, a test indicating bilateral distal occlusion was confirmed at laparoscopy with a high degree of accuracy. In contrast, radiographic studies suggesting alternate types of tubal disease were not as accurate, with only 63% of the findings confirmed at laparoscopy. In women with a completely normal HSG, the test accurately predicted the presence of patent Fallopian tubes with a false negative rate of only 3.6%. However, over 40% of women with a normal HSG had associated pelvic disease (adhesions or endometriosis) detected at the time of laparoscopy.
A sample is collected from the husband after masturbation preferably after 3 days of abstinence. In WHO 2010, the new normal values are based on data from men with proven fertility, men who were known to help their partners conceive in the previous 12 months. Following a large analysis of semen parameters from over 4000 men in 14 countries, a new set of 5th percentile parameters was recommended. Below are the comparisons of the old and new
reference values:
- Parameter WHO 1999 WHO 2010
- Volume 2 ml 1.5 ml
- Concentration 20 million/ml 15 million/ml
- Progressive motility 50% 32%
- Normal forms 14% 4%
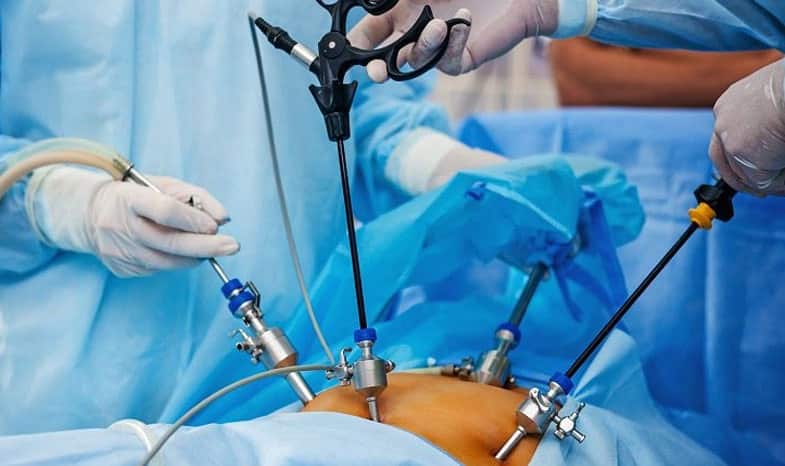
Laparoscopy is a surgical procedure that involves insertion of a narrow telescope-with 3 or 5mm instruments in the abdomen and allows evaluation of the abdominal and pelvic organs including the area of the uterus, fallopian tubes and ovaries.
It helps us to detect whether the tubes are healthy and patent or not .If the tubes are blocked then they can be made patent by hysteroscopic cannulation with the additional help of hysteroscopy.
It also helps us to confirm, diagnose endometriosis and thereby treat it by fulguration and enucleation of chocolate cysts in the ovaries.It helps us to confirm and remove fibroids( tumours of the uterus).Because of the cost and invasive nature of laparoscopy it should not be the first test in the couples diagnostic evaluation. In general, semen analysis, hysterosalpingogram, assessment of ovarian reserve and documentation of ovulation should be assessed prior to consideration of laparoscopy.
My plan will focus on answering many important questions, including the following:
- Are you ovulating?
- Are your fallopian tubes normal?
- Is your uterus receptive to implantation?
- Are the sperm normal in number and function?
FEMALE
Day 3 Bloodwork
A clinician will perform bloodwork on day 3 of your menstrual cycle to test levels of the following:
- E2 (estrogen): the main female reproductive hormone secreted from the ovary.
- FSH (follicle-stimulating hormone): releases from the brain and stimulates the ovary to mature an egg. High FSH levels can indicate to your physician that the hypothalamus and pituitary glands are working harder than normal due to a decrease in ovarian reserve (egg supply). FSH levels can vary from cycle to cycle.
- AMH (anti-Müllerian hormone): AMH is the most accurate predictor of a woman’s egg supply. This test can be more accurate than FSH because there is no fluctuation from month to month and the test is not dependent on a woman’s menstrual cycle, which means women can have the test at any point.
- AMH: The Best Predictor of Current Female Fertility
- LH (luteinizing hormone): a hormone that is integral to the final maturation and release of a mature follicle.
Internal Baseline Ultrasound
Embryos implant in the uterus, which makes it necessary to perform tests to determine if a woman’s uterine cavity is normal. A sonographer or physician will perform an ultrasound of the ovaries between days 2 through 4 of your cycle. We use this test to determine the antral follicle count (AFC), which represents the number of eggs available for pregnancy that month.
MALE
Semen Analysis
The test results will tell your physician the number of sperm in your semen (your sperm count), whether they are normal (morphology), and how well they swim (motility).
So in my opinion, if you have any such issues, please feel free to consult me. I don’t believe in a lot of investigations.With very few investigations, we can get your treatment going, answer all your queries, and help you achieve a successful pregnancy.Most of the times, people are misguided by quacks,and people who do not have any idea about infertility.So inthis era of IUI, IVF and IVF ICSI etc, it is very very likely that you will have a baby in your arms.Whenever you come for a consultation, try to meet your fertilty specialist in empty stomach as soon as your periods end, ie., around day 8 to day 10 menses with your partner having around 2 days of abstinence to get your investigations and treatment going. Also don’t forget to bring all your previous papers so that you don’t have to repeat those tests again.
- DON’T HESITATE TO CONSULT ME IF YOU HAVE BEEN TRYING FOR A BABY FOR MORE THAN A YEAR .IF YOU ARE MORE THAN 35 YEARS OLD AND IF YOUR HUSBAND IS MORE THAN 40 YEARS OLD, THEN MEET ME IF YOU HAVE TRIED CONTINUOUSLY FOR ONLY 6 MONTHS.
- DON’T IGNORE IF YOU HAVE INFERTILITY DUE TO PCOD OR ENDOMETRIOS.DON’T FEEL DISHEARTENED ALSO BECAUSE BOTH THESE CONDITIONS CAN BE TREATED AND MONITORED.
- DON’T JUMP TO PROCEDURES LIFE IVF IMMEDIATELY WITHOUT PROPER INVESTIGATIONS AND TREATMENT PROTOCOLS.REMEMBER:EVEN IVF DOESN’T HAVE 100 PERCENT SUCCESSS RATES.
- DON’T BE UNDER THE IMPRESSION THAT EVALUATION OF INFERTILITY REQUIRES AN ARRAY OF COSTLY INVESTIGATIONS.IT CAN BE ASSESSED WITH MINIMAL TESTS AND COST.